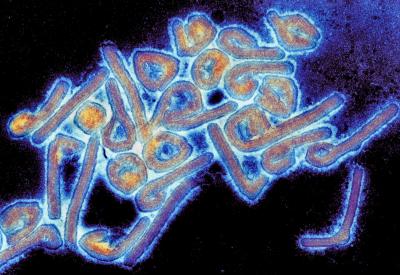
Marburg Hemorrhagic Fever is a viral disease native to Africa that causes severe bleeding, organ failure and sometimes death. It is caused by the Marburg virus, which is found on animal hosts and passed on through contact from them to humans. After the initial contact, the virus can spread to other humans through contaminated needles and bodily fluid. The disease occurs in sporadic outbreaks of which the fatality ranges from 24 to 88 percent of cases in one specific outbreak. Large outbreaks in Marburg and Frankfurt, Germany and Belgrade, Serbia in 1967 led to the initial recognition of the illness and were associated with lab experiments involving African green monkeys from Uganda. However, it is now believed that African fruit bats are the original hosts of the Marburg virus.
In earlier years, spread of the disease to humans was mostly due to prolonged exposure to caves and mines with fruit bat inhabitants. Now, the main way of transmission is through contact with contaminated needles and bodily fluids of the infected. Infection through medical equipment is associated with a faster, more severe case with a higher chance of fatality. Certain burial rites that involve close contact with the deceased also play a role in transmission. Health care workers also contract Marburg through close contact with patients without good infection control procedures in place.
The incubation period, the time between infection and onset of symptoms, for Marburg can be between two and 21 days. The symptoms begin suddenly with a high fever, malaise and headaches. Muscle aches and pains are also fairly common in beginning symptoms. Diarrhea, abdominal pain and cramping, nausea and vomiting can begin from the third day of symptoms. At this point, patients are described as having a “ghost-like” appearance, with deep set eyes and severe lethargy. During the European outbreaks in 1967, a non-itchy rash was also noted as a common symptom for patients. The patients who develop hemorrhaging, or severe bleeding, will usually do so between five and seven days of the first recognition of symptoms. Fatal cases commonly have severe bleeding as one of the symptoms seen. The bleeds can be from the gums, nose, venepuncture sites that are used to draw blood from patients for tests and in vomit and feces. During the last and most severe phase of Marburg, patients have a constant high fever and an affected central nervous system that results in confusion, irritability and aggression. For fatal cases, death has been reported about eight to nine days after symptoms start, preceded by great blood loss.
Marburg hemorrhagic fever can only be diagnosed with lab tests using tests such as the enzyme-linked immunosorbent assay, antigen detection tests, serum neutralization tests, reverse transcriptase PCR assay and virus isolation by cell culture. These tests have a great biohazard risk and are only performed under maximum containment measures. Severe cases require supportive care as patients are in constant need of fluids or electrolytes due to the blood loss. There are no specific treatments or vaccines for the Marburg virus, so all care at the moment is preventative in terms of contact awareness and palliative care for those infected. New drug therapies are being developed and may be approved in the future as effective treatments.